Jump to: How do we measure the reversal of type 2 diabetes? | How do we achieve remission? | So does significant weight loss ‘cure’ type 2 diabetes? | Can everyone achieve remission? | Exceptions to the rule | Take home message
Type 2 diabetes reversal: The bottom line
- Type 2 diabetes can’t be ‘cured’ per se, but it can be reversed for some people.
- Significant weight loss seems to be the most effective way to achieve remission, as suggested by the results of the DiRECT study.
- Once in remission, it’s essential to maintain the weight loss, otherwise type 2 diabetes will most likely return.
- This is due to fat accumulation in the pancreas killing insulin-producing cells (pancreatic beta cells).
- If these cells are damaged beyond repair then achieving remission would not be possible, hence why not everyone with type 2 diabetes can go into remission.
- Some rare forms of diabetes get mistaken for type 2 diabetes, but remission is not possible in these cases.
Type 2 diabetes is characterised by the body’s poor ability to respond to insulin (insulin resistance).
Insulin is the hormone responsible for regulating blood sugar levels. When we say ‘blood sugar’ we mean ‘blood glucose’.
Both terms are used interchangeably. Reduced insulin sensitivity results in consistently high blood sugar.
If blood sugar levels are consistently high, there’s an increased risk of developing type 2 diabetes.
This is usually known as ‘prediabetes’ (a.k.a impaired glucose tolerance). You can think of blood glucose levels as a continuum, with prediabetes and type 2 diabetes being points along the spectrum.
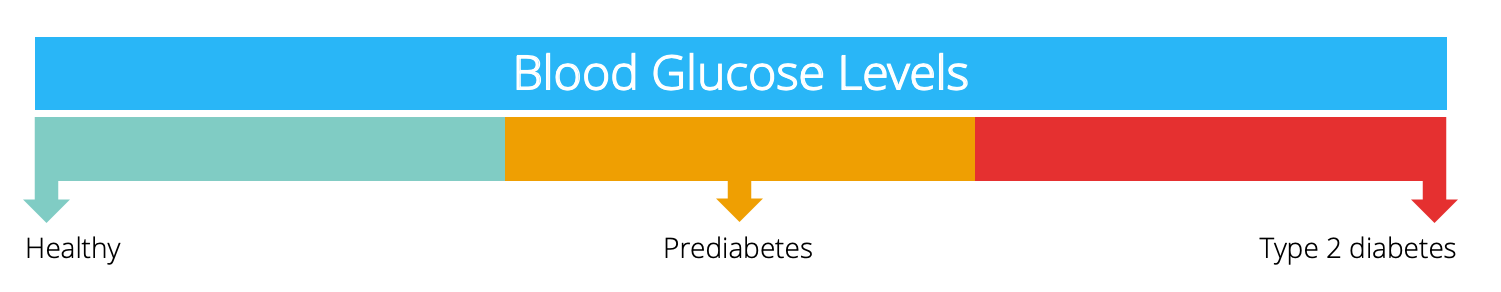
Rather than ‘curing’ type 2 diabetes, recent research has suggested that the condition can be reversed for some people following extensive weight loss.
For individuals where this is possible, moving from the ‘type 2 diabetes point’ on the spectrum towards the healthy blood glucose point.
Medication-assisted weight loss with a future focus
Start with Wegovy or Mounjaro, transition to habit-based health with our support


How do we measure the reversal of type 2 diabetes?
The usual marker of having reversed type 2 diabetes is when the condition is put into remission. There is some debate about the exact definition of remission. Diabetes UK defines remission as meeting these three criteria:
- Weight loss
- HbA1c levels at less than 48mmol/mol on two venous blood tests within 6 months
- Achieving the above after coming off all diabetes medications.
HbA1c (glycated haemoglobin) refers to red blood cells with glucose attached.
HbA1c levels are used because our blood glucose levels constantly change throughout the day based on when/what we eat and physical activity.
Taking a one-off blood sugar measurement at a specific time doesn’t help diagnose type 2 diabetes.
When the body can’t use glucose properly, as with type 2 diabetes, it sticks to the red blood cells and circulates through our blood vessels.
Since red blood cells have an average life of 3-4 months, HbA1c helps us to see the average blood glucose levels over a 2-3 month period.
For an individual with type 2 diabetes, the aim is to A) get into remission and B) get HbA1c levels as close to the healthy range as possible.
| No Diabetes | Prediabetes | Type 2 Diabetes | Remission | |
| Description | When an individual has healthy blood glucose levels. |
The transition between healthy blood glucose levels and diabetes, where blood sugar levels are higher than usual. |
Consistently high blood glucose levels. Serious complications if untreated. |
When an individual diagnosed with type 2 diabetes exhibits healthy blood glucose levels over an extended period. |
| A1c Diagnosis Criteria (mmol/mol) | < 42 | 42 ≤ 47 | ≥ 48 | < 48 |
| Reversible | n/a | Yes | Yes, if caught early enough and there’s not been too much damage to the pancreas. | n/a |
It is worth noting that the table above is a rough guide that can be useful for diagnosis, but it is still possible to have type 2 diabetes with an HbA1c level below 48 mmol/mol.
Key points:
- Successfully reversing type 2 diabetes is known as going into remission.
- HbA1c levels are a good indication of blood glucose levels over time.
- The aim with type 2 diabetes is to go into remission and then move as close to a healthy HbA1c level as possible.
How do we achieve remission?
Significant weight loss appears to be the most effective way to achieve type 2 diabetes remission.
Professor Roy Taylor, a leading researcher of type 2 diabetes, and colleagues at Newcastle University conducted the first-ever dietary and lifestyle intervention trial with remission as the primary endpoint. This was called the DiRECT study.
320 participants, all diagnosed with type 2 diabetes within the last six years, were randomised into either the intervention group or the control group.
The intervention was a very low-calorie diet programme. Participants dramatically reduced their energy intake to 850 calories a day and were slowly reintroduced to a regular, healthy diet to maintain weight loss.
The control group received the usual treatment on the NHS for type 2 diabetes.
This study is ongoing, but the results have demonstrated that after one year, those in the intervention group lost significantly more body weight (average of 10 kg) than the control group (average of 1kg).
In addition, 46% of the intervention group went into remission, compared to only 4% in the control group.
At two years, 36% of those who began the trial in the intervention group were in remission, as opposed to 3% in the control group.
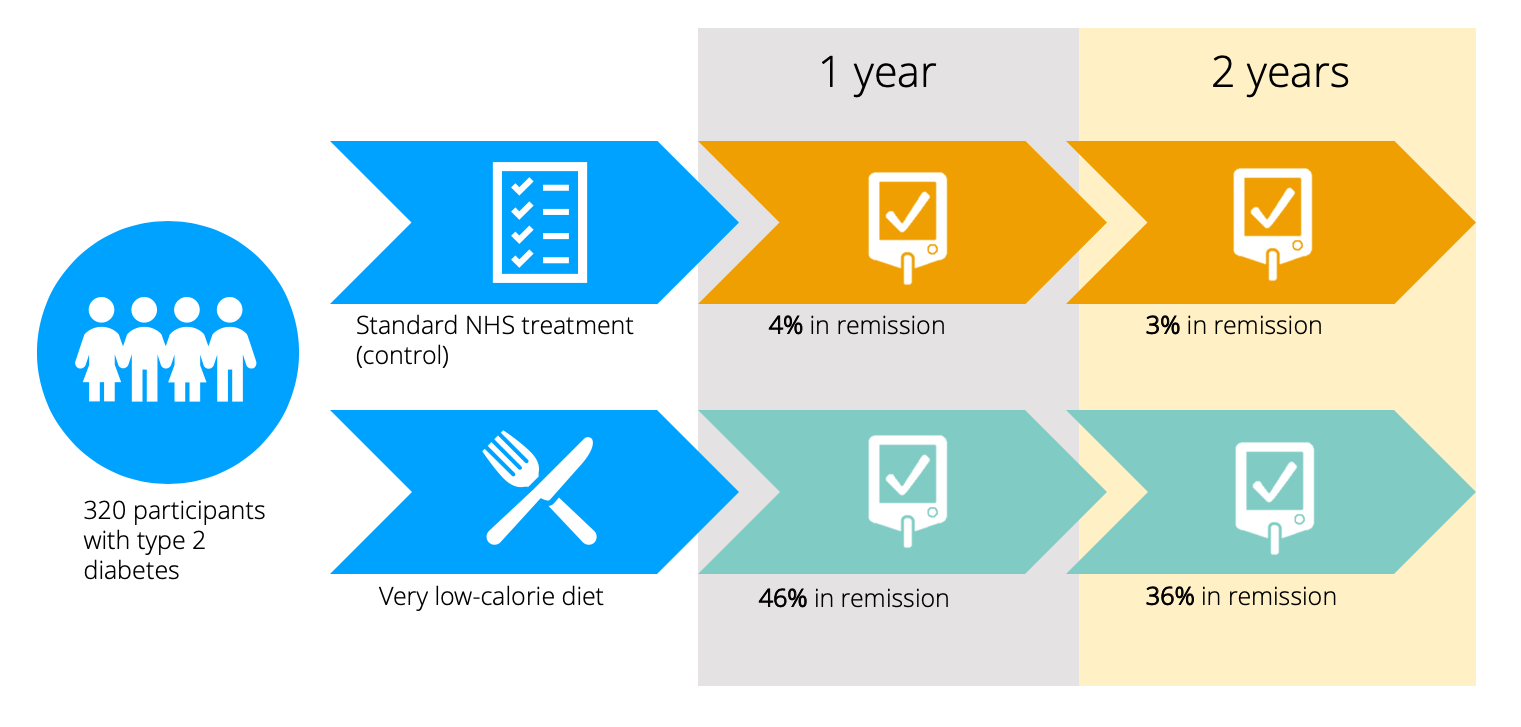
These results suggest that significant weight loss can reverse type 2 diabetes and result in regular insulin activity for some, even if the individual has been diagnosed up to 10 years ago.
The DiRECT study placed participants on a low-calorie shake diet to achieve significant weight loss.
This diet dramatically reduced overall energy intake. Although effective in the short term, we don’t think low-calorie shakes are the easiest, healthiest, most cost-effective, or most sustainable approach to weight loss.
This approach doesn’t teach people how to live healthily, only that there is a short-term fix that can be applied.
Our understanding of the scientific literature is that it’,s far more effective in the long term to achieve weight loss and remission through healthy lifestyle and behaviour change.
Key points:
- For the majority of people, significant weight loss appears to be the most effective way to achieve remission of type 2 diabetes.
- The DiRECT study, which is the first randomised trial to examine remission as the main endpoint, supports this.
So, does significant weight loss ‘cure’ type 2 diabetes?
The simple answer is no. Type 2 diabetes can’t be ‘cured’, but evidence suggests that significant weight loss can reverse the condition in some people.
Once in remission, it’s essential to maintain weight loss. Otherwise, type 2 diabetes will return.
Professor Taylor suggests a mechanism for how type 2 diabetes occurs, which explains why failing to maintain weight loss in remission leads back to diabetes:
- Overeating leads to excess fat in the liver.
- The liver responds poorly to insulin and adds more glucose to the blood.
- Excess fat in the liver is passed on to the pancreas, causing insulin-producing cells (pancreatic beta cells) to stop working.
- Losing weight reduces fat inside the pancreas.
- This re-starts the insulin-producing cells, resulting in the normal production of insulin.
- Weight gain takes you back to step 1.
Professor Taylor’s key point is that everyone has a ‘personal fat threshold’.
To go into remission (and stay in remission), you must lose enough weight (and maintain this weight loss) below your personal threshold. In his own words:
‘Some people can tolerate a Body Mass Index (BMI) of 40 or more without getting type 2 diabetes.
Others cannot tolerate a BMI of 22 without diabetes appearing, as their bodies are set to function normally at a BMI of, say 19. This is especially so in people of South Asian ethnicity.’
Key points:
- Type 2 diabetes cannot be ‘cured’, but drastic weight loss can reverse the condition for some people.
- Overeating leads to fat in the liver and pancreas, which kills insulin-producing cells (pancreatic beta cells).
- Everyone has a personal fat threshold, which is how much fat the body can tolerate before developing type 2 diabetes.
Can everyone achieve remission?
Some people can’t achieve remission despite losing weight below their personal threshold.
Professor Taylor acknowledges that a reduction in liver and pancreas fat depends on pancreatic beta cells’ ability to recover.
If these cells are damaged beyond repair, perhaps from having type 2 diabetes for a very long time, then significant weight loss is unlikely to reverse diabetes successfully.
In his prize-winning lecture about the pathology of diabetes, Professor Roger Unger suggests that the build-up of fat in the pancreas causes ceramide to accumulate in the pancreas.
Ceramide is toxic and kills pancreatic beta cells. It’s possible that having type 2 diabetes long enough (10 years plus) without treating it leads to too many pancreatic beta cells getting destroyed by this process.
This means that even if individuals lose weight below their personal fat threshold, they cannot go into remission.
This highlights the individual variability of type 2 diabetes and the complex systems at play when we talk about reversing it or going into remission.
This could partly explain why not all of the participants in the DiRECT study who lost a significant amount of weight went into remission.
Perhaps some participants didn’t lose enough weight to reach below their personal fat threshold, and those that did but didn’t achieve remission possibly had irresolvable pancreatic damage.
Key points:
- Not everyone with type 2 diabetes can achieve remission.
- This may be because too many pancreatic beta cells have been damaged beyond repair.
- This is more likely the longer someone has had type 2 diabetes.
Exceptions to the rule
Professor Taylor caveats that this research is relevant for individuals with the ‘usual’ type 2 diabetes. Rare forms of diabetes exist that can easily be mistaken for type 2 diabetes, including:
A) ‘Pancreatic’ diabetes
This occurs after several cases of pancreatitis and is likely caused by pancreas damage.
B) ‘Monogenic’ diabetes
This genetic form of diabetes is commonly found in slim individuals diagnosed in early adulthood with a family history of diabetes.
C) Slow onset type 1 diabetes
Sometimes type 1 diabetes develops slowly, appearing in adulthood, and these individuals usually need insulin therapy soon after being diagnosed.
Key points:
- Three rare forms of diabetes often get mistaken for type 2 diabetes.
- These forms cannot achieve remission.
Take home message
- Type 2 diabetes can’t be ‘cured’ per se, but it can be reversed for some people.
- Significant weight loss seems to be the most effective way to achieve remission, as suggested by the results of the DiRECT study.
- Once in remission, it’s essential to maintain weight loss. Otherwise, type 2 diabetes will most likely return.
- This is due to fat accumulation in the pancreas killing insulin-producing cells (pancreatic beta cells).
- If these cells are damaged beyond repair, then remission would not be possible, hence why not everyone with type 2 diabetes can go into remission.
- Some rare forms of diabetes get mistaken for type 2 diabetes, but remission is impossible in these cases.