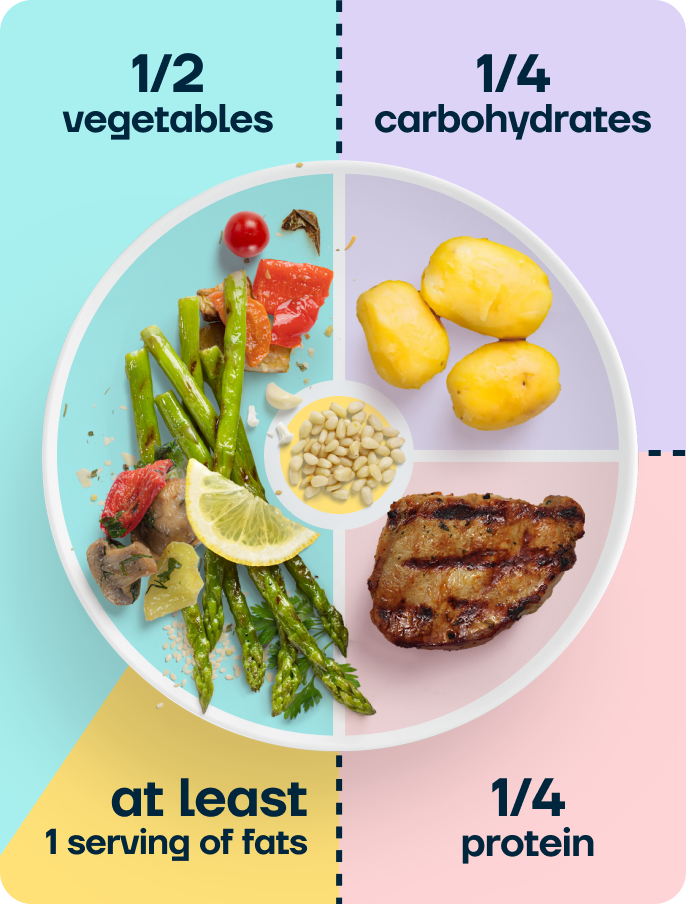What is osteoarthritis?
Osteoarthritis (OA) is a condition where the protective cartilage covering the ends of bones gradually wears down. This leads to pain, stiffness, and reduced mobility in affected joints.
It most commonly affects the knees, hips, hands, and spine. Symptoms tend to develop gradually and can include pain during or after movement, morning stiffness, joint swelling, and reduced range of motion.
Women face a higher risk of developing OA than men, particularly after the age of 50.
The decline in oestrogen during menopause affects cartilage health and inflammation levels, which partly explains this difference.
Common symptoms include:
- Joint pain during or after movement
- Stiffness, especially in the morning or after sitting for a while
- Swelling around the joints
- A grating sensation when moving the joint
- Loss of flexibility
How weight affects your joints
The relationship between body weight and osteoarthritis works through two connected pathways.
Understanding both helps explain why weight management is important for joint health, though it isn’t the only factor.
Mechanical stress on joints
Every additional kilogram of body weight increases the force on knee joints by two to three times during everyday activities like walking and climbing stairs.2
Research shows that for every 5 kg of weight gain, the risk of developing knee osteoarthritis increases by 36%.2 This is why knees and hips, which bear the most load, are the joints most commonly affected.
Inflammation from body fat
Body fat isn’t just stored energy. It’s a metabolically active tissue that releases inflammatory compounds into the bloodstream, including proteins like leptin, IL-6, and TNF-alpha.
These compounds, if released in excess, increase inflammation throughout the body and can contribute to cartilage breakdown over time. This helps explain why osteoarthritis can also affect non-weight-bearing joints, such as the hands.
The value of maintaining a stable weight
A 2023 study found that maintaining a stable weight from young adulthood through midlife reduced the risk of developing arthritis by 74% compared to people who gained significant weight during this period.3
However, body composition matters as much as total weight. Having more muscle mass and exercising regularly protects joints by providing better support and stability around them.
This is why any approach to weight loss should aim to preserve muscle through adequate protein and regular movement, rather than focusing on the number on the scales alone.
What is Mounjaro?
Mounjaro is a prescription weight-loss injection containing the drug tirzepatide. It’s taken once a week.
It works by mimicking two gut hormones, GLP-1 and GIP, that communicate with the brain’s appetite control centre (the hypothalamus) to reduce hunger and food-seeking behaviour.
Mounjaro also slows the rate at which food moves through the stomach. This means you feel full sooner and stay satisfied for longer after eating.
In clinical trials, people taking Mounjaro achieved an average weight loss of up to 26% after 88 weeks of treatment.4
Mounjaro supports weight loss through two mechanisms:
- Reducing appetite by acting on the brain’s hunger signals
- Slowing digestion so you feel full for longer
Mounjaro and osteoarthritis
A 2024 retrospective study compared osteoarthritis outcomes across different anti-obesity medications.
It found that people taking tirzepatide (Mounjaro) had a 43% lower risk of developing osteoarthritis compared to those taking semaglutide (Ozempic or Wegovy).1
The study included over 39,000 people with obesity and followed them for six months.
Overall, people using any anti-obesity medication had a 27% lower risk of osteoarthritis compared to people not using medication.1
These findings are observational, which means they show an association rather than proving that Mounjaro directly prevents osteoarthritis.
But the size of the difference is notable and likely reflects the combined effect of significant weight loss and reduced inflammation.
What this could mean for existing osteoarthritis
No clinical trials have yet tested Mounjaro specifically in people with existing osteoarthritis.
However, the weight loss it supports could help in several ways:
- Reducing the mechanical load on weight-bearing joints
- Lowering systemic inflammation that contributes to cartilage damage
- Improving mobility, which makes it easier to exercise and strengthen the muscles around joints
An ongoing registered trial called STOP Knee OA is investigating the effect of tirzepatide in people with obesity and knee osteoarthritis.1 Results aren’t yet available, but the trial could provide more direct evidence in the future.
Protecting muscle and bone during weight loss
Rapid weight loss can sometimes reduce muscle mass and bone density.
For people with osteoarthritis, preserving both is important for joint stability and long-term mobility.
To reduce this risk while taking Mounjaro:
- Lose weight slowly at a sustainable rate of 0.5 to 1kg per week
- Include protein at every meal to support muscle maintenance
- Incorporate some form of strength or resistance exercise
- Ensure adequate calcium and vitamin D intake
- Work with your healthcare team to monitor your progress
| Finding |
Detail |
Source |
| OA risk reduction with tirzepatide vs semaglutide |
43% lower risk |
Luo et al. (2024), retrospective cohort1 |
| OA risk reduction with any anti-obesity medication vs none |
27% lower risk |
Luo et al. (2024), retrospective cohort1 |
| Average weight loss with Mounjaro |
Up to 26% at 88 weeks |
SURMOUNT-4 trial, JAMA (2023)4 |
| Knee OA risk per 5 kg weight gain |
36% increased risk |
Zheng & Chen (2015), systematic review2 |
| OA risk with stable weight from young adulthood to midlife |
74% lower risk vs significant weight gain |
Zhang et al. (2023), retrospective cohort3 |
Foods that support joint health
What you eat can influence inflammation levels, bone strength, and how well your body maintains and repairs cartilage.
For people living with osteoarthritis, there are a few nutrition tips to consider:
Protein for muscle maintenance
Strong muscles support and stabilise joints. When you’re losing weight, getting enough protein helps preserve muscle mass while your body reduces fat stores.
Good sources include chicken, turkey, fish, eggs, Greek yoghurt, tofu, beans, and lentils. Aim to include a source of protein at every meal.
Omega-3 fats for inflammation
Omega-3 fatty acids have anti-inflammatory properties that may help manage osteoarthritis symptoms.
A 2023 meta-analysis of nine trials found that omega-3 supplementation significantly reduced pain in people with OA compared to placebo.5
Oily fish like salmon, mackerel, sardines, and trout are the richest dietary sources. Aim for two portions per week. Walnuts, chia seeds, and flaxseeds also contain omega-3, though in a form the body converts less efficiently.
Along with dietary sources, omega-3 supplementation is also safe and effective for lowering inflammation in the body. Speak to your GP about potentially adding these to your daily meals.
Calcium and vitamin D for bones
Calcium is essential for bone strength, and vitamin D helps the body absorb it. Both are important for people with osteoarthritis, especially if you’re losing weight and want to protect bone density.
Good calcium sources include dairy products, tinned sardines (with bones), fortified plant milks, broccoli, and kale.
For vitamin D, spending time outdoors helps in the summer months, and a supplement is recommended in the UK during autumn and winter.
Vegetables and complex carbohydrates
Vegetables provide antioxidants that help manage inflammation. Leafy greens like spinach and kale, as well as colourful vegetables like peppers, tomatoes, and beetroot, are particularly rich in these compounds.
Complex carbohydrates provide sustained energy and fibre, which support gut health and can help regulate inflammation.
Good options include rolled oats, brown rice, sweet potato, quinoa, beans and lentils, and wholegrain or sourdough bread.
A balanced approach
Rather than focusing on individual foods, your overall dietary pattern is the most important factor.
A useful framework is the balanced plate: fill half your plate with vegetables, a quarter with protein, a quarter with complex carbohydrates, and add a serving of healthy fat.
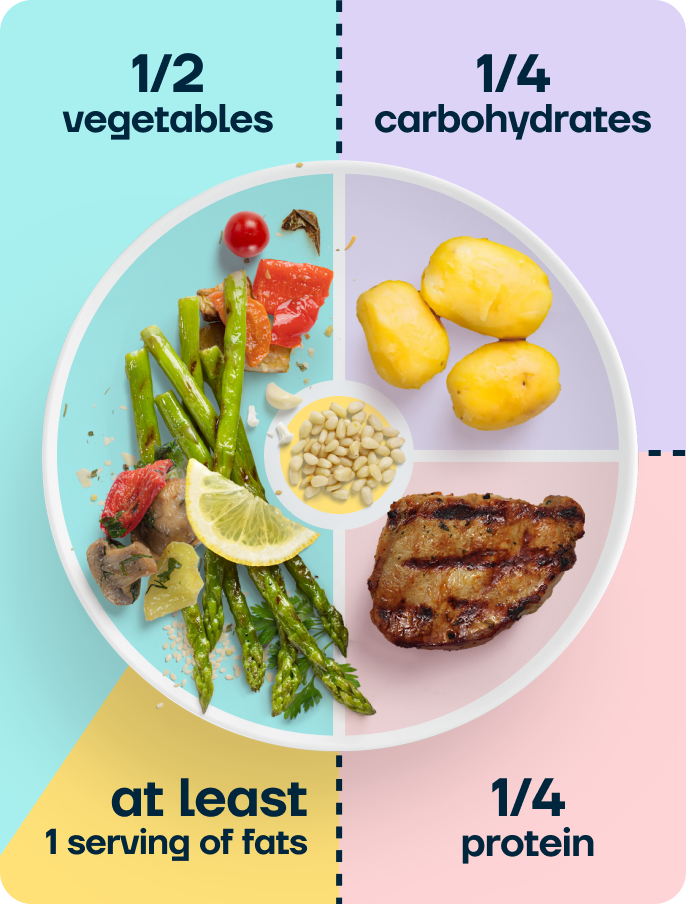
Managing reduced appetite on Mounjaro
Mounjaro can significantly reduce your appetite, so it’s important to prioritise nutrient-dense foods when you do eat.
Focus on protein and vegetables first, then add complex carbohydrates and fat. Smaller, more frequent meals may be easier to manage than three large ones if nausea is an issue in the early weeks.
Staying active with osteoarthritis
When your joints are painful, the idea of exercise can feel counterintuitive. But regular movement is one of the most effective ways to manage osteoarthritis symptoms, and any amount is better than none.
We’d recommend starting small and building consistency rather than trying to hit a specific target from day one.
Research on habit formation suggests that linking a new behaviour to an existing routine, like a short walk after dinner, helps it become automatic over time.6
Joint-friendly movement
Low-impact activities are generally easier on joints while still providing real benefits. Options include:
- Walking, starting with whatever distance feels comfortable
- Swimming or water-based exercise, where buoyancy reduces joint loading
- Cycling (stationary or outdoor), which keeps joints moving without heavy impact
- Gentle yoga or tai chi for flexibility and balance
A systematic review of aquatic exercise for OA found it was effective for reducing pain, improving joint function, and improving quality of life.7 The warm water in pool-based exercise can also help relax muscles and ease stiffness.
Building strength around your joints
Strength training is particularly valuable for people with osteoarthritis.
Stronger muscles absorb more of the load during movement, reducing the stress on your joints.
You don’t need a gym to start. Bodyweight exercises like sit-to-stands from a chair, wall press-ups, or step-ups on a low step can build strength gradually. Resistance bands are another accessible option.
As it feels manageable, you can gradually do a little more. The NHS recommends aiming for 150 minutes of moderate activity per week, but this is a long-term goal, not a starting point.
When to be cautious
Some discomfort during exercise is normal with osteoarthritis, but sharp or worsening pain is a signal to stop or modify what you’re doing.
If a particular activity consistently increases your pain, speak to your GP or a physiotherapist about alternatives.
Living with chronic pain
Osteoarthritis doesn’t just affect your joints. Living with chronic pain can take a significant toll on mood, energy, and quality of life.
A systematic review found that around 20% of people with osteoarthritis experience symptoms of depression, and a similar proportion experience symptoms of anxiety.8 That’s roughly one in five people.
How pain and mood are connected
Chronic pain can reduce your ability to do things you enjoy, disrupt sleep, and make it harder to stay physically active. Over time, this can lead to a cycle where reduced activity worsens both pain and mood.
Pain also affects the brain directly. Persistent pain can alter how the brain processes emotions, making people more susceptible to low mood and anxiety.8
Reduced mobility and isolation
When moving is painful, it’s natural to do less. But withdrawing from activities and social situations can increase feelings of isolation and loneliness, particularly for older adults.
Finding ways to stay connected, whether through adapted activities, online communities, or regular contact with friends and family, can make a meaningful difference.
When to speak to your GP
If you’re finding that pain is affecting your mood, sleep, or ability to engage with daily life, it’s worth raising this with your GP.
Depression and anxiety are treatable, and addressing them can also improve how you manage your osteoarthritis.
Psychological support, whether through talking therapies, peer support groups, or self-management programmes, can help alongside physical treatments.
Frequently asked questions
Can Mounjaro help with osteoarthritis pain?
Mounjaro hasn’t been directly tested for osteoarthritis pain relief.
However, the weight loss it supports can reduce the mechanical load on joints and lower inflammation, both of which contribute to OA pain.
A trial called STOP Knee OA is currently investigating this question more directly.
Is Mounjaro safe to take if you have osteoarthritis?
Yes. There are no known interactions between Mounjaro and osteoarthritis or its treatments.
The main consideration is protecting muscle mass and bone density during weight loss, which you can support by consuming adequate protein and engaging in regular exercise.
How much weight do you need to lose to improve osteoarthritis symptoms?
Research suggests that even a 5-10% reduction in body weight can meaningfully reduce joint pain and improve function in people with knee osteoarthritis.
Every kilogram lost reduces the load on your knee joints by two to three times that amount during walking.
Will exercise make my osteoarthritis worse?
In most cases, no. Regular, appropriate exercise is one of the best things you can do for osteoarthritis.
It strengthens the muscles that support your joints, improves flexibility, and can reduce pain over time.
Low-impact activities like swimming, cycling, and walking are good starting points.
What foods should I avoid if I have osteoarthritis?
There’s no need to eliminate entire food groups. However, diets high in ultra-processed foods, refined carbohydrates, and excess sugar can increase inflammation.
Focusing on whole foods, vegetables, protein, and omega-3-rich fish is a more helpful approach than focusing on the foods you ‘shouldn’t’ eat.
Can omega-3 supplements help with osteoarthritis?
A 2023 meta-analysis found that omega-3 supplementation can reduce pain in people with osteoarthritis.5 Eating oily fish twice a week is the best dietary approach.
If you’re considering supplements, speak to your GP or pharmacist about the right dose.
Does Mounjaro affect bone density?
Rapid weight loss from any cause can reduce bone density. This isn’t specific to Mounjaro, but it’s an important consideration if you have osteoarthritis.
Eating enough protein, getting adequate calcium and vitamin D, and including some resistance exercise can all help protect your bones during weight loss.
Can I take anti-inflammatory painkillers alongside Mounjaro?
There are no known interactions between Mounjaro and common OA pain relievers such as paracetamol or ibuprofen.
However, Mounjaro slows gastric emptying, which can affect how quickly oral medications are absorbed. Always discuss your full medication list with your prescriber.
How long does it take for weight loss to improve osteoarthritis symptoms?
Many people notice improvements in joint pain and mobility within the first few months of losing weight.
The benefits tend to increase as weight loss continues. Combining weight loss with regular exercise typically produces better outcomes than either approach alone.
Take home message
Mounjaro can be taken safely if you have osteoarthritis, and the weight loss it supports may reduce joint pain by lowering both mechanical stress and inflammation.
A 2024 study found a 43% lower risk of developing OA in people taking tirzepatide compared to semaglutide.1
Protecting muscle mass and bone density during weight loss is important.
Prioritising protein, omega-3-rich foods, calcium, and vitamin D in your diet, alongside regular movement, gives your joints the best chance of benefiting from the weight you lose.
How Second Nature can help
Second Nature combines medication with a structured habit-change programme built around the balanced plate model: half vegetables, a quarter protein, a quarter complex carbohydrates, plus a serving of healthy fat.
A published study in JMIR Formative Research found that members using Second Nature’s semaglutide-supported programme achieved an average weight loss of 19.1% at 12 months, with 77.7% losing at least 10% of their body weight.9
Second Nature's Mounjaro and Wegovy programmes
Second Nature provides Mounjaro or Wegovy as part of our Mounjaro and Wegovy weight-loss programmes.
Why choose Second Nature over other medication providers, assuming you're eligible?
Because peace of mind matters.
We've had the privilege of working with the NHS for over eight years, helping people across the UK take meaningful steps toward a healthier, happier life.
Our programmes are designed to meet people where they are, whether that means support with weight loss through compassionate one-to-one health coaching, or access to the latest weight-loss medications (like Mounjaro and Wegovy) delivered alongside expert care from a multidisciplinary team of doctors, psychologists, dietitians, and personal trainers.
At the heart of everything we do is a simple belief: real, lasting change comes from building better habits, not relying on quick fixes. We're here to support that change every step of the way.
With over a decade of experience, thousands of lives changed, and a long-standing record of delivering programmes used by the NHS, we believe we're the UK's most trusted weight-loss programme.
We hope to offer you something invaluable: peace of mind, and the support you need to take that first step.
References
- Luo et al. (2024). The impact of approved anti-obesity medications on osteoarthritis. Expert Opinion on Pharmacotherapy.
- Zheng & Chen (2015). Body mass index and risk of knee osteoarthritis: systematic review and meta-analysis of prospective studies. BMJ Open.
- Zhang et al. (2023). Relationship of weight change patterns from young to middle adulthood with incident rheumatoid arthritis and osteoarthritis. Frontiers in Endocrinology.
- Aronne et al. (2024). Continued treatment with tirzepatide for maintenance of weight reduction in adults with obesity: the SURMOUNT-4 randomised clinical trial. JAMA.
- Deng et al. (2023). Effect of omega-3 polyunsaturated fatty acids supplementation for patients with osteoarthritis: a meta-analysis. Journal of Orthopaedic Surgery and Research.
- Lally et al. (2010). How are habits formed: modelling habit formation in the real world. European Journal of Social Psychology.
- Song et al. (2022). Effects of aquatic exercises for patients with osteoarthritis: systematic review with meta-analysis. Healthcare.
- Stubbs et al. (2016). Prevalence of depressive symptoms and anxiety in osteoarthritis: a systematic review and meta-analysis. Age and Ageing.
- Richards et al. (2025). Real-world effectiveness of a digitally delivered GLP-1 RA-supported weight management programme. JMIR Formative Research, 9(1), e72577.