Can you take Wegovy after a gastric band?
Wegovy isn’t specifically advised against after a gastric band.
The Wegovy SmPC lists previous gastrointestinal surgery as a reason for caution rather than as an absolute contraindication.1
A gastric band creates a narrow passage between the upper and lower stomach. Semaglutide slows gastric emptying, so food stays in the stomach for longer.2
Combining these two effects increases the risk of nausea, vomiting, and food getting stuck at the band site.
Whether the band is still in place, has been deflated, or has been removed changes how your prescriber will approach treatment.
With the band still in place and inflated, the priority is to monitor for excessive restriction.
If the band has been deflated or removed, your prescriber will follow the standard Wegovy dose schedule, with extra attention to your nutritional intake given your bariatric history.
Your prescriber will likely start at the lowest dose (0.25 mg weekly) and increase slowly, monitoring how you tolerate the combination.
If your band is still in place, they may also ask you to discuss band adjustment with your bariatric team before starting.
How gastric bands work
A gastric band is an adjustable silicone ring placed around the top of the stomach.
It creates a small pouch above the band that fills quickly, so you feel full after eating less food.3
The band is adjusted via a port under the skin, usually on the abdominal wall.
Saline is injected into the port to tighten the band or removed to loosen it, meaning the level of restriction can change over time.3
The band doesn’t alter the hormones that influence hunger and fullness.
A sleeve gastrectomy or gastric bypass changes our gut hormone balance, increasing GLP-1 and PYY levels after meals. A gastric band doesn’t. It simply narrows the opening so food passes through more slowly.
Because the band relies entirely on restriction, it’s the most reversible bariatric procedure.
It’s also the procedure with the weakest long-term outcomes for weight maintenance, which is why many people explore additional options like Wegovy after years with a band in place.
Why weight regain happens after a gastric band
Weight regain after a gastric band is common.
A 2019 systematic review and meta-analysis of long-term bariatric surgery outcomes found that gastric banding had the weakest sustained weight loss among major bariatric procedures, with high rates of revisional surgery over 10 to 20 years of follow-up.4
First, the band doesn’t address the hormones that influence our appetite.
Your body still produces the same levels of ghrelin (the hunger hormone) as before surgery.
Over time, hunger signals often intensify due to lower energy intake rather than ease.
Second, the band itself can develop problems.
Slippage occurs when the band moves from its original position, reducing its effectiveness.
Erosion happens when the band gradually wears through the stomach wall.
Port disconnection or infection can make adjustments impossible.3
Third, many people learn to ‘eat around’ the band. Soft, calorie-dense foods like chocolate, crisps, and ice cream pass through the restriction easily.
Bread, fibrous vegetables, and lean meat are more likely to get stuck, so people sometimes avoid the very foods that would support their health.
A significant number of bands are eventually removed.
Once removed, the surgical support is gone, and weight regain often accelerates without additional support.
How Wegovy works differently from a gastric band
Wegovy contains semaglutide, which mimics a hormone called GLP-1 (a hormone our gut naturally produces after eating that signals fullness to the brain).2
Semaglutide acts on appetite centres in the brain, reducing hunger and food cravings.
It also slows gastric emptying, so food stays in the stomach longer and you feel satisfied for longer after eating.2
The STEP 1 trial showed that people taking semaglutide 2.4 mg lost an average of 14.9% of their body weight over 68 weeks, compared to 2.4% with placebo.6
This study was conducted in people without prior bariatric surgery, so the figure isn’t directly applicable to someone with a band, but it still gives a sense of the medication’s effect on appetite-driven weight loss.
For people with a history of bariatric surgery, the 2024 Obesity Reviews meta-analysis cited above found that GLP-1 receptor agonists produced meaningful additional weight loss with an acceptable safety profile.5
The difference is that Wegovy reduces hunger directly by acting on brain appetite signals.
A gastric band can’t do that; it only limits how much food the stomach can hold.
For someone whose band isn’t providing adequate restriction, or whose band has been removed, semaglutide could provide more long-term support for weight loss.
Should the band be deflated or removed before starting Wegovy?
This is one of the most common questions for people considering Wegovy with a gastric band still in place.
There isn’t a single right answer; the decision depends on your band’s current status, how much fluid is in it, whether you’ve had complications, and what your bariatric team recommends.
Leave the band as it is
If your band is currently providing useful restriction without complications, your team may suggest leaving it in place and starting semaglutide at a low dose with close monitoring. This is sometimes the preferred approach for people whose band is working but who haven’t reached their weight goal.
Deflate the band partially or fully
Removing some or all of the saline reduces mechanical restriction. This is often preferred over surgical removal because it’s reversible: the band can be re-inflated later if needed.
Some bariatric teams routinely recommend deflation before starting a GLP-1 medication, particularly if the band is currently tight or has caused vomiting.
Remove the band surgically
If the band has caused complications such as slippage, erosion, or chronic dysphagia, removal is usually necessary regardless of medication plans.
Once the band is out, semaglutide is prescribed in much the same way as for someone without a bariatric history.
Who should make the decision
This decision should be made with the bariatric surgical team that placed or has been managing your band, rather than a GLP-1 prescriber alone.
If you’re under NHS bariatric follow-up, your specialist clinic can advise.
If you had your band privately and have lost contact with the surgeon, your GP can refer you to a local bariatric service for assessment.
Safety considerations
The combination of a gastric band and semaglutide raises specific safety considerations that don’t apply to the same extent as those for other bariatric procedures.
Nausea and vomiting
Nausea is the most common side effect of semaglutide, affecting around 44% of people in the STEP 1 trial.6
With a gastric band in place, there’s an additional mechanical cause for nausea if food can’t pass through the restricted opening efficiently.
Frequent vomiting can cause the band to slip from its position, which may require surgical correction or removal.3
If you’re experiencing regular vomiting after starting Wegovy, contact your bariatric team.
Band adjustment
Your surgeon may recommend deflating the band before starting semaglutide, or at least reviewing the current fill level.
Because semaglutide slows gastric emptying independently, the combined effect with a tight band can be excessive.1
Food texture
People with a gastric band already know that certain food textures cause problems.
Dry bread, tough meat, and fibrous vegetables can get stuck at the band site.
Semaglutide’s effect on gastric emptying can make this worse, so chewing thoroughly, eating easier-to-digest meals, and eating slowly help reduce the risk of food getting stuck.
Nutritional monitoring
Both the gastric band and semaglutide reduce food intake. When combined, the reduction may be significant enough to affect your nutritional status.
Regular blood tests should check vitamin and mineral levels, particularly iron, vitamin B12, vitamin D, and calcium.8
If you’ve had bariatric surgery, you should already be on lifelong supplementation, including a complete multivitamin, vitamin B12, iron, and calcium with vitamin D.
Starting Wegovy doesn’t change those supplement requirements.
Reduced food intake means less is coming in from your diet, so consistent supplement intake helps prevent deficiencies.8
Gastric band vs other bariatric procedures with Wegovy
| Factor |
Gastric band |
Gastric sleeve |
Gastric bypass |
| Mechanism |
Mechanical restriction only |
Restriction plus increased gut hormone (GLP-1, PYY) release |
Restriction, malabsorption, and increased gut hormone release |
| Effect on GLP-1 |
No change |
Increased postprandial GLP-1 |
Significantly increased postprandial GLP-1 |
| Long-term weight maintenance |
Weakest of the three; high revisional surgery rates over 10 to 20 years4 |
Better sustained weight loss than the band |
Best long-term outcomes |
| Reversibility |
Fully reversible |
Irreversible |
Technically reversible but rarely done |
| Procedure-specific complications |
Slippage, erosion, port issues3 |
Reflux, leak risk |
Dumping syndrome, internal hernia |
| Key concern with Wegovy |
Vomiting and band slippage; delayed gastric emptying combined with restriction |
Reduced stomach volume combined with delayed gastric emptying |
Altered drug absorption; dumping syndrome risk |
| Why someone might add Wegovy |
Hormonal appetite drivers untouched by the band; high regain rates |
Weight regain as initial hormonal effects diminish |
Weight regain, though less common than after a band |
Foods to focus on
Adding Wegovy to a band changes how much food you can comfortably eat and how quickly food moves through your stomach.
You may need to be more careful about food choices than someone on Wegovy without a band.
Protein first
Getting enough protein is a priority after any bariatric procedure.
With reduced food intake from both the band and semaglutide, you need to get enough protein, vitamins, and minerals from smaller portions than you used to eat.
A palm-sized portion of protein at each meal is a practical guide.

With a band, the texture of your protein affects how easily it passes through.
Mince, fish, eggs, Greek yoghurt, and slow-cooked meat tend to pass through more comfortably than dry chicken breast or tough steak. Beans and lentils are also good options and add fibre.
Managing reduced appetite on Wegovy
Semaglutide significantly reduces appetite, and when combined with a gastric band, you may be able to manage only very small portions.
Prioritise nutrient-dense foods that are easier to digest, like soups, stews, casseroles, and other one-pot dishes like bolognese or curry, rather than trying to eat more volume.
If you’re struggling to meet your nutritional needs, aim for three smaller meals a day with protein-rich snacks in between.
A small pot of Greek yoghurt with fruit or a handful of nuts (chewed thoroughly) between meals can help fill the gap.
The balanced plate
Second Nature’s balanced plate model is a practical framework: half vegetables, a quarter protein, a quarter complex carbohydrates, plus a serving of healthy fat.
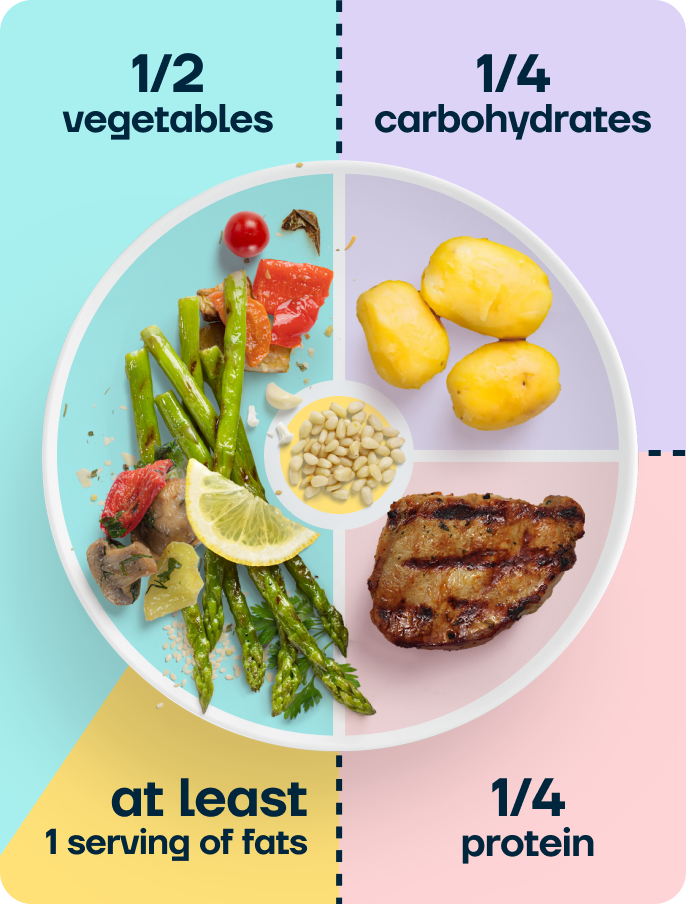
Cooked vegetables tend to be easier to tolerate with a band than raw salad leaves, and softer carbohydrates like rolled oats or sweet potato are usually more comfortable than dry bread.
You may not manage a full plate, but keeping these proportions helps ensure you’re getting a good balance from whatever you do eat.
Physical activity
Consistent activity helps preserve muscle mass during weight loss and improves cardiovascular fitness, whether or not it supports weight loss.
A meta-analysis of 22 randomised controlled trials found that structured exercise programmes improved body composition in people who’d had bariatric surgery.7
Starting with what you can do
If you’re not currently active, start with something small that fits into your day. A 10-minute walk after dinner is a realistic starting point.
Research on habit formation shows that linking a new behaviour to an existing routine makes it more likely to stick.9
Gradually do more as it feels manageable. The goal is to build a consistent pattern that you can sustain.
Aerobic activity
Walking, cycling, swimming, and dancing are all low-impact and easy to build into a routine.
Swimming is particularly worth considering after bariatric surgery because it doesn’t put pressure on the abdomen.
Anything that gets you slightly out of breath gives a cardiovascular benefit.
Resistance training
Resistance training helps preserve lean muscle mass during weight loss. This is particularly relevant when you’re losing weight through both a band and semaglutide, since rapid weight loss can lead to muscle loss alongside fat loss.7
You don’t need a gym membership. Bodyweight exercises like squats, wall press-ups, and standing up from a chair without using your hands are effective starting points. Resistance bands are another affordable option.
Band-specific considerations
If your band is still in place, intense core exercises or heavy lifting could potentially affect the port site.
Speak to your bariatric team about any precautions specific to your situation.
If you experience nausea during exercise, which can happen on semaglutide, try exercising before meals rather than after, and keep intensity moderate until you know how your body responds.
Mental health after bariatric surgery
Disordered eating patterns, including loss-of-control eating and grazing, are common after bariatric procedures and can contribute to weight regain.11
With a gastric band specifically, the relationship with food can become complicated.
Certain foods get stuck, eating too quickly causes pain, and social situations around food can become stressful.
Some people develop anxiety around eating or begin avoiding social meals altogether.
Body image after weight regain
Weight regain after bariatric surgery often brings shame and a sense of having failed something that was supposed to be permanent.
Many people withdraw from support services and become reluctant to seek further help.
If this sounds familiar, it’s worth knowing that weight regain after a gastric band is extremely common and isn’t a personal failure.
The band has the weakest long-term outcomes among bariatric procedures because it doesn’t address the underlying causes of weight gain.4
Where to find support
Your GP can refer you for psychological support if you’re experiencing anxiety, low mood, or disordered eating patterns related to your weight or bariatric history.
Many bariatric services offer psychological support as part of their follow-up care.
Cognitive behavioural therapy (CBT) has good evidence for helping people manage the psychological challenges of living with obesity and disordered eating after bariatric surgery.11
When to speak to your GP
Contact your GP or bariatric team if you experience any of the following while taking Wegovy with a gastric band:
- Persistent vomiting, which could indicate the band is too tight or has slipped
- Difficulty swallowing or food frequently getting stuck
- Severe or worsening nausea that doesn’t improve with dose adjustments
- Signs of dehydration (dark urine, dizziness, dry mouth)
- Abdominal pain near the port site
- Symptoms of nutritional deficiency (fatigue, hair loss, tingling in hands or feet)
- Low mood, anxiety, or disordered eating patterns affecting your daily life
- Any concerns about how the medication is interacting with your band
If your band has been removed and you’re taking Wegovy, the standard side effect monitoring applies.
The most common side effects are gastrointestinal: nausea, diarrhoea, constipation, and vomiting.1
Frequently asked questions
Is Wegovy safe to take with a gastric band still in place?
It can be, but it requires medical supervision.
The combination of the band’s physical restriction and semaglutide’s effect on gastric emptying increases the risk of nausea and vomiting.
Your bariatric team may recommend deflating the band or adjusting the fill level before starting treatment.1
Can I take Wegovy if my gastric band has been removed?
Yes. Once the band is removed, the stomach typically returns to its normal shape and function.
Wegovy is prescribed in much the same way as for someone without a bariatric history, though your prescriber should still be aware of your surgical history given the ongoing nutritional considerations.5
Why didn’t my gastric band work long-term?
The band works purely through mechanical restriction and doesn’t change the hormonal signals that drive hunger.
Over time, the body adapts to the restriction, and soft, high-calorie foods can bypass it, leading to complications like slippage or erosion.34
Will Wegovy help me lose the weight I regained after having my band removed?
Evidence suggests it can. A 2024 systematic review and meta-analysis found that GLP-1 receptor agonists produced meaningful weight loss in people who had regained weight after bariatric surgery, with semaglutide outperforming liraglutide.5
Individual results vary, and medication works best when combined with diet and lifestyle changes.
Do I need to change what I eat when starting Wegovy with a band?
You may need to be more careful with food textures and portion sizes, as the combined effect of the band and semaglutide reduces the amount of food your stomach can comfortably handle.
Prioritise protein, chew thoroughly, and eat slowly. Cooked vegetables are usually easier to tolerate than raw ones.
How does Wegovy compare to having my band replaced or converted to a sleeve?
Revision surgery is a major operation with its own risks.
Wegovy is a non-surgical option that reduces hunger by acting on brain appetite signals, whereas the band doesn’t.
Your bariatric team can help you weigh up the options based on your specific situation.5
Can I exercise normally with a gastric band and Wegovy?
Yes, though check with your bariatric team about restrictions around the port site. Start with low-impact activity and build up gradually.
Nausea from semaglutide can affect exercise tolerance, so try exercising before meals if this is an issue.
How long will I need to take Wegovy?
How long you need to take Wegovy depends on how much weight you need to lose and whether you need long-term support from the medication to maintain lower hunger levels.
Wegovy is currently licensed for long-term use. Research shows that when people stop taking semaglutide, most of the weight lost is regained within a year.10
Still, emerging research shows that if you develop healthy habits while on the medication, you’re less likely to regain weight after stopping.
Your prescriber will discuss the long-term plan with you, which should include building sustainable dietary and exercise habits alongside the medication.
Is weight regain after a gastric band my fault?
No. Weight regain after a gastric band is common and well-documented.
The band has the weakest long-term outcomes among bariatric procedures because it only addresses restriction, not the root causes of weight gain.4
Seeking additional support through medication is a practical next step, not a sign of failure.
Will my GP prescribe Wegovy if I’ve already had bariatric surgery?
NHS prescribing of Wegovy under NICE TA875 requires you to be under specialist weight management services (Tier 3) and meet specific BMI criteria.12
Many people with a bariatric history are already linked into specialist services, which can make eligibility assessment more straightforward.
If NHS access isn’t available, private prescribers can also assess eligibility, including providers experienced in post-bariatric weight regain.
Your GP or bariatric follow-up team can advise on the options available to you.
Take home message
You can take Wegovy after a gastric band, but the combination needs medical supervision.
The band works purely through physical restriction and doesn’t change the hormonal signals that influence our appetite, which is why weight regain is so common.
Wegovy works differently, reducing appetite through brain signalling and slowing gastric emptying.
If the band is still in place, your bariatric team will need to monitor for increased nausea and vomiting risk and may recommend deflation before starting treatment.
For people whose band has been removed, Wegovy offers hormonal appetite support that the band never provided.
Whatever your situation, the medication works best alongside structured diet and behavioural support. Without that, weight regain after stopping is common.10
Second Nature’s medicated weight-loss programme combines GLP-1 medication with support from registered dietitians and a structured habit-change programme.
A 2025 study published in JMIR Formative Research found that active subscribers on Second Nature’s semaglutide-supported programme lost an average of 19.1% of their body weight at 12 months, with 77.7% achieving at least 10% weight loss.13
The programme is built around the balanced plate model: half vegetables, a quarter protein, a quarter complex carbohydrates, plus a serving of healthy fat.
Second Nature's Mounjaro and Wegovy programmes
Second Nature provides Mounjaro or Wegovy as part of our Mounjaro and Wegovy weight-loss programmes.
Why choose Second Nature over other medication providers, assuming you're eligible?
Because peace of mind matters.
We've had the privilege of working with the NHS for over eight years, helping people across the UK take meaningful steps toward a healthier, happier life.
Our programmes are designed to meet people where they are, whether that means support with weight loss through compassionate one-to-one health coaching, or access to the latest weight-loss medications (like Mounjaro and Wegovy) delivered alongside expert care from a multidisciplinary team of doctors, psychologists, dietitians, and personal trainers.
At the heart of everything we do is a simple belief: real, lasting change comes from building better habits, not relying on quick fixes. We're here to support that change every step of the way.
With over a decade of experience, thousands of lives changed, and a long-standing record of delivering programmes used by the NHS, we believe we're the UK's most trusted weight-loss programme.
We hope to offer you something invaluable: peace of mind, and the support you need to take that first step.
References
- Electronic Medicines Compendium. (2024). Wegovy 2.4 mg solution for injection in pre-filled pen – Summary of Product Characteristics.
- Drucker, D.J. (2018). Mechanisms of action and therapeutic application of glucagon-like peptide-1. Cell Metabolism, 27(4), 740-756.
- Shen, X. et al. (2015). Long-term complications requiring reoperations after laparoscopic adjustable gastric banding: a systematic review. Surgery for Obesity and Related Diseases, 11(4), 956-964.
- O’Brien, P.E. et al. (2019). Long-term outcomes after bariatric surgery: a systematic review and meta-analysis of weight loss at 10 or more years for all bariatric procedures and a single-centre review of 20-year outcomes after adjustable gastric banding. Obesity Surgery, 29(1), 3-14.
- Esparham, A. et al. (2024). Safety and efficacy of glucagon-like peptide-1 (GLP-1) receptor agonists in patients with weight regain or insufficient weight loss after metabolic bariatric surgery: a systematic review and meta-analysis. Obesity Reviews, 25(11), e13811.
- Wilding, J.P.H. et al. (2021). Once-weekly semaglutide in adults with overweight or obesity (STEP 1). New England Journal of Medicine, 384(11), 989-1002.
- Bellicha, A. et al. (2021). Effect of exercise training before and after bariatric surgery: a systematic review and meta-analysis. Obesity Reviews, 22 Suppl 4, e13296.
- Mechanick, J.I. et al. (2020). Clinical practice guidelines for the perioperative nutrition, metabolic, and nonsurgical support of patients undergoing bariatric procedures. Obesity, 28(4), O1-O58.
- Lally, P. et al. (2010). How are habits formed: modelling habit formation in the real world. European Journal of Social Psychology, 40(6), 998-1009.
- Wilding, J.P.H. et al. (2022). Weight regain and cardiometabolic effects after withdrawal of semaglutide: the STEP 1 trial extension. Diabetes, Obesity and Metabolism, 24(8), 1553-1564.
- Conceição, E.M. et al. (2022). Disordered eating after bariatric surgery: clinical aspects, impact on outcomes, and intervention strategies. Current Obesity Reports.
- NICE. (2023). Semaglutide for managing overweight and obesity (TA875).
- Richards, R. et al. (2025). A remotely delivered GLP-1RA-supported specialist weight management program in adults living with obesity: retrospective service evaluation. JMIR Formative Research, 9, e72577.